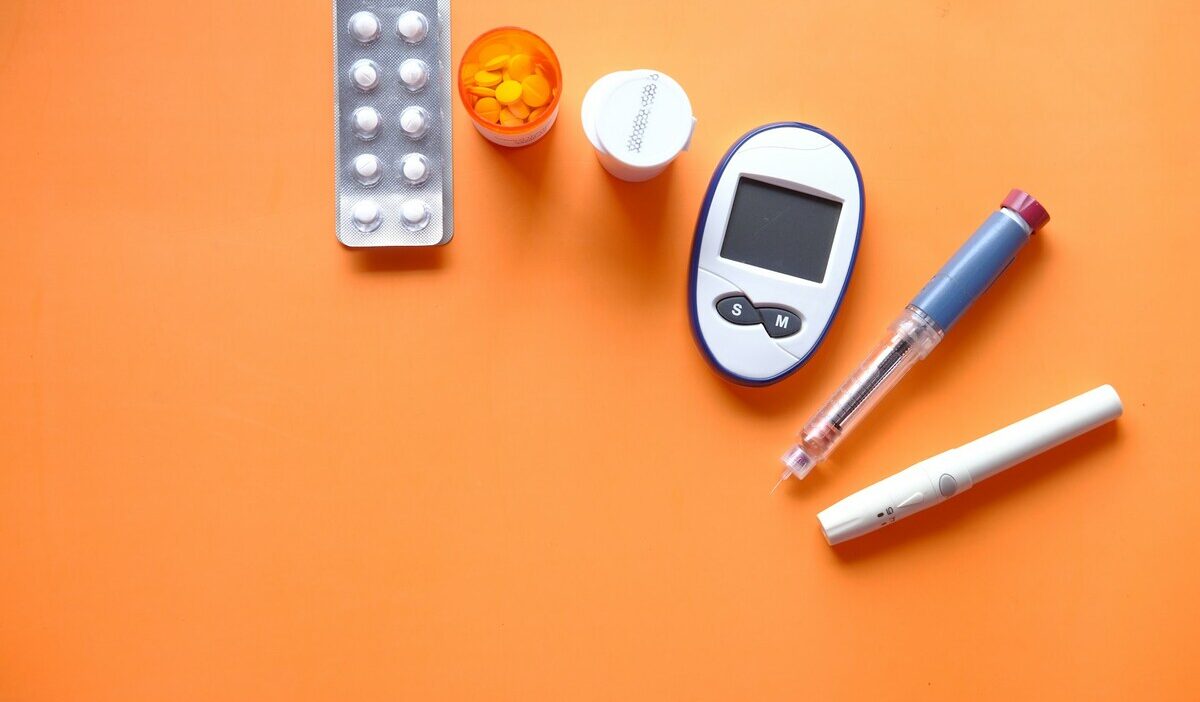
Managing diabetes requires consistent monitoring, medication, and access to specialized medical equipment.
Because these supplies can be expensive, many people rely on Medicaid to help cover the costs. This leads to a common question: What diabetic supplies are covered by Medicaid?
In this guide, we’ll explain what diabetic supplies are covered by Medicaid, how coverage works, and how patients can obtain these supplies through their Medicaid plan.
What Diabetic Supplies Are Covered By Medicaid?
Medicaid typically covers a wide range of supplies needed to monitor and manage diabetes. These supplies are considered medically necessary for individuals diagnosed with diabetes and prescribed by a healthcare provider.
Common supplies covered by Medicaid often include:
- Blood glucose monitoring equipment
- Insulin and injection supplies
- Continuous glucose monitoring systems
- Certain diabetes-related medications
Although the specific items covered may vary by state, these core supplies are generally included in most Medicaid programs.
Blood Glucose Meters And Test Strips
One of the most important tools for managing diabetes is a blood glucose meter, which measures blood sugar levels.
Medicaid usually covers blood glucose monitoring equipment, including:
- Blood glucose meters
- Test strips
- Lancets
- Lancing devices
These supplies allow patients to monitor blood sugar levels throughout the day.
Coverage may include a certain number of test strips per month, depending on the patient’s treatment plan and medical needs. Patients who use insulin may be approved for more frequent testing supplies.
Insulin, Syringes, And Pen Needles
Another important category when asking what diabetic supplies are covered by Medicaid includes insulin and injection supplies.
Medicaid commonly covers:
- Insulin medications
- Syringes
- Pen needles
- Insulin delivery pens
Because insulin is essential for many people with diabetes, it is typically included in Medicaid prescription coverage when prescribed by a doctor.
Some Medicaid programs may also cover multiple types of insulin depending on the patient’s medical needs and treatment plan.
Continuous Glucose Monitors (CGMs) And Sensors
Continuous Glucose Monitors (CGMs) are advanced devices that track glucose levels throughout the day and night.
Many Medicaid programs now cover CGM systems when medically necessary. These devices may include:
- CGM transmitters
- Sensors
- Receivers or compatible monitoring devices
CGMs can provide real-time glucose readings and alerts when blood sugar levels become too high or too low.
However, Medicaid may require documentation from a healthcare provider to demonstrate that the device is medically necessary.
>>>Read more: Does Medicaid Cover NIPT Test? State Coverage Explained
Does Medicaid Cover Insulin Pumps And CGM Devices?
Some patients require advanced diabetes management tools such as insulin pumps or specialized CGM systems. Coverage for these devices may be available but often involves additional approval steps.
Prior Authorization Requirements
For certain devices like insulin pumps or advanced CGM systems, Medicaid may require prior authorization.
Prior authorization means that the healthcare provider must submit documentation explaining why the device is medically necessary.
This process may involve:
- A detailed treatment history
- Evidence that other treatments were ineffective
- Documentation showing that the patient would benefit from the device
If Medicaid approves the request, the device and related supplies may be covered.
Brand And Model Restrictions
Even when Medicaid covers insulin pumps or CGM systems, there may be restrictions on which brands or models are included.
Some Medicaid plans maintain a list of approved devices and manufacturers. Patients may be required to use equipment from those approved lists.
In some cases, healthcare providers can request an exception if a specific device is medically necessary for the patient.
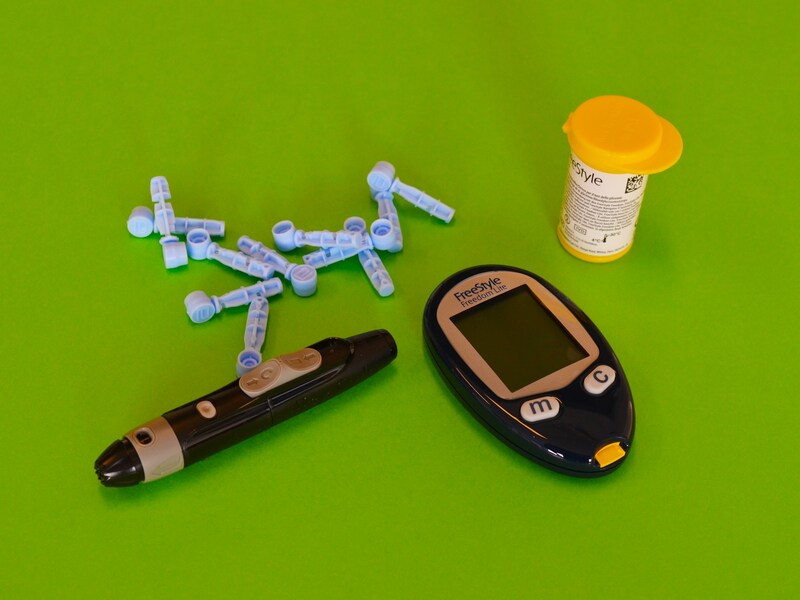
How Medicaid Coverage Varies By State
Although Medicaid is funded by both federal and state governments, individual states manage their own programs.
Because of this, the answer to what diabetic supplies are covered by Medicaid may vary depending on where a patient lives.
Some states may:
- Cover a wider range of diabetes technology
- Provide larger quantities of testing supplies
- Offer additional diabetes education programs
- Other states may have stricter requirements for device approval.
Patients should review their state Medicaid benefits or speak with a healthcare provider to understand what supplies are covered under their specific plan.
>>>Read more: Does Medicaid Pay For Liposuction? What You Need To Know in 2026
How To Get Diabetic Supplies Through Medicaid
Once a patient qualifies for Medicaid coverage, obtaining diabetic supplies usually involves working with a healthcare provider and an approved pharmacy or supplier.
Prescription And Doctor Documentation
Most diabetic supplies covered by Medicaid require a prescription from a doctor or healthcare provider.
The provider typically determines:
- Which supplies are medically necessary
- How frequently are the supplies needed
- The appropriate devices for the patient’s condition
The prescription is then submitted to the pharmacy or medical supplier that works with Medicaid.
Approved Pharmacies And Medical Suppliers
Patients receiving Medicaid coverage must usually obtain supplies through approved pharmacies or durable medical equipment suppliers.
These suppliers handle the billing directly with Medicaid and ensure that the patient receives covered items.
Some patients may receive supplies through:
- Local pharmacies
- Mail-order medical supply companies
- Durable medical equipment providers
Using approved suppliers helps ensure that the supplies are covered and reduces out-of-pocket costs.
FAQs
Does Medicaid Cover All Test Strips?
Medicaid usually covers blood glucose test strips, but the number of strips allowed each month may depend on the patient’s treatment plan and whether insulin is used.
Are CGMs Fully Covered By Medicaid?
In many cases, Medicaid may cover Continuous Glucose Monitor systems if they are considered medically necessary. However, approval may require documentation and may be limited to specific devices or suppliers.
Conclusion
Understanding what diabetic supplies are covered by Medicaid can help patients manage their condition more effectively while reducing financial stress.
In most cases, Medicaid covers essential diabetes management supplies such as blood glucose meters, test strips, insulin, syringes, and continuous glucose monitoring devices. More advanced equipment, like insulin pumps, may also be covered when medically necessary and approved.
Because Medicaid programs vary by state, patients should check their specific state guidelines and consult their healthcare provider to confirm which supplies are covered.
With proper documentation and prescriptions, Medicaid can help ensure that individuals with diabetes have access to the tools they need to monitor and manage their health.