Does Medicaid pay for dental implants? For most enrollees, the honest answer is no. Dental implants are considered a premium restorative procedure, and most state Medicaid programs classify them as elective rather than medically necessary.
This guide covers why Medicaid rarely covers implants, when approval is possible, and what your options are if coverage is denied – including a closer look at Idaho, Virginia, and New York.
Does Medicaid Pay For Dental Implants?
In most cases, Medicaid does not pay for dental implants.
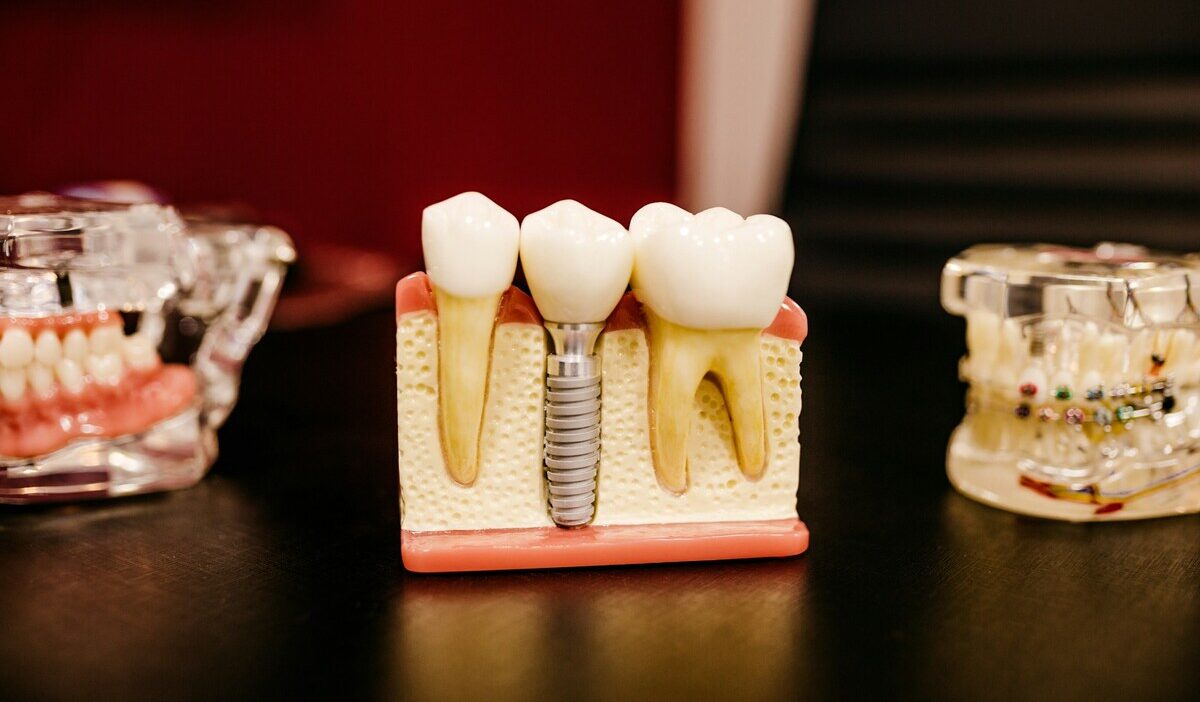
Implants are a permanent tooth replacement option that involves surgically placing a titanium post into the jawbone, topped with a crown.
Because of the cost and complexity involved, most state Medicaid programs exclude them from the list of covered dental services.
States are only required to provide emergency dental care for adults under federal Medicaid rules. Adult dental benefits beyond emergencies, including implants, are optional. Even states with comprehensive adult dental coverage tend to draw the line at implants.
Why Dental Implants Are Rarely Covered Under Medicaid
Medicaid programs operate under tight budgets and prioritize essential, cost-effective care.
Dental implants typically cost between $3,000 and $6,000 per tooth, making them one of the most expensive dental procedures available.
From Medicaid’s perspective, less expensive alternatives, such as dentures or bridges, achieve the same functional outcome of replacing a missing tooth.
As a result, most state programs consider implants a non-essential upgrade rather than a medically required treatment.
Additionally, implants require multiple appointments over several months, involve oral surgery, and are not reversible if complications arise.
These factors make state Medicaid administrators unlikely to include them as a standard covered benefit.
When Medicaid Might Cover Dental Implants as Medically Necessary
There are limited situations where Medicaid may consider dental implants medically necessary:
- Congenital conditions: Patients born with missing teeth due to conditions like ectodermal dysplasia may have a stronger case for implant coverage.
- Jaw reconstruction after cancer: If implants are required as part of reconstructive care following oral cancer treatment, Medicaid may cover them under medical rather than dental benefits.
- Traumatic injury: Severe facial trauma that makes conventional prosthetics non-functional may support a medical necessity claim.
- Inability to tolerate dentures: In rare cases, documented physical inability to wear dentures due to bone loss or anatomical issues has supported implant approvals.
These exceptions are not guaranteed and vary by state. A formal prior authorization request with detailed clinical documentation is required in all cases.
>>> Read more: Does Medicaid Cover Invisalign? Coverage Rules & 4 Steps
What to Do If Medicaid Denies Your Dental Implant Request
A denial is not always final. If Medicaid rejects your implant request, you have options:
- Request a formal appeal; every Medicaid program has an appeals process. Ask your plan for the appeal form and deadlines.
- Get a letter of medical necessity from your dentist or oral surgeon detailing why implants are the only clinically appropriate option.
- Ask your primary care physician to support the claim if the tooth loss is connected to a medical condition or treatment.
- Explore state ombudsman or patient advocacy services for help navigating the appeals process.
The Medicaid.gov appeals information page outlines your rights as an enrollee when a service is denied.
Does Medicaid Cover Dental Implants for Adults?
For adults specifically, Medicaid dental implant coverage is extremely rare. Adult dental benefits under Medicaid are optional, and even states that offer comprehensive adult dental care almost universally exclude implants in favor of dentures or bridges.
Adults seeking implants through Medicaid face a higher burden of proof than children. They must typically demonstrate that no other tooth replacement option is clinically viable and provide extensive documentation from multiple providers.
Adult Dental Coverage vs Children Under 21
Children under age 21 enrolled in Medicaid receive dental coverage through the Early and Periodic Screening, Diagnostic and Treatment (EPSDT) program.
Under EPSDT, states must cover any dental service that is medically necessary, regardless of whether that service appears on the state’s standard adult benefit list.
This means a child or young adult under 21 with a documented need for a dental implant, such as a congenitally missing tooth, has a much stronger chance of getting coverage approved than an adult over 21.
Dentists working with pediatric Medicaid patients can submit a medical necessity request directly tied to EPSDT requirements.
For adults over 21, no such federal mandate exists. Coverage is entirely at the state’s discretion, which is why implant approvals for adults are so uncommon.
States That May Cover Implants When Medically Necessary
A more detailed look at the answer for does Medicaid pay for dental implants is that a small number of states have broader adult dental benefit structures that leave room for implant coverage in exceptional cases.
These tend to be states with comprehensive adult dental Medicaid programs, such as New York and Illinois.
Even in these states, implants are not a standard benefit. Coverage depends on individual case review, prior authorization, and proof that alternatives are not appropriate.
Most approvals come through reconstructive situations or medical pathways rather than standard dental benefits.
>>> Read more: Does Aspen Dental Take Medicaid? 2026 Easy Explain
Idaho Coverage for Dental Implant
For anyone wondering does Idaho Medicaid cover dental implants, the coverage situation is fairly limited.
Idaho’s adult dental benefits are structured around essential care like emergency extractions and basic restorative procedures, and implants fall outside of what’s currently covered for adult enrollees.
Children have more options here. EPSDT opens up broader dental coverage for younger patients, and individual cases involving medical necessity can sometimes be reviewed separately.
For adults, though, the more realistic path tends to be dentures or partials rather than implants. If affordability is the main concern, Idaho’s community health centers do offer dental services on a sliding fee scale, which can make a real difference.
Reaching out to your local Medicaid office is also a good step to confirm what your specific plan includes, since benefit details can vary.
Dental Implant Coverage in Virginia
Virginia is worth looking at a little more closely compared to Idaho, because the state has actually expanded its adult dental benefits in recent years.
So if you’re researching does Virginia Medicaid cover dental implants, it helps to know that Virginia’s Cardinal Care program now covers a broader range of services than many states, including exams, cleanings, fillings, and extractions. Even so, implants haven’t been included as a standard benefit.
For patients under 21, EPSDT does allow for implant coverage when there’s a documented medical need, which is meaningful. Adult enrollees aren’t entirely without options either.
If your dentist believes your case has strong clinical grounds, submitting a prior authorization request with thorough documentation is a reasonable step to take.
It isn’t guaranteed, but it’s a legitimate path that some patients have had success with.
>>> Read more: Does Medicaid Cover Wisdom Teeth Removal? States Easy Guide
New York’s Dental Implant Coverage
New York tends to have one of the more comprehensive adult dental Medicaid programs in the country, so it can be surprising to find that the answer to does Medicaid cover dental implants in NY is still largely no for most adults.
The state covers quite a lot, including exams, cleanings, fillings, root canals, extractions, and dentures, which already puts it well ahead of states like Idaho in terms of scope.
Implants are treated differently, though. In reconstructive situations, particularly following oral cancer treatment, they may be considered through medical rather than dental benefits.
That’s a specific exception rather than a general rule, but it’s worth knowing about.
For those who have been denied coverage, New York has a structured appeals process that’s genuinely worth pursuing if your main goal, looking for support for does Medicaid pay for dental implants, hasn’t changed.
Dental schools affiliated with institutions like NYU and Columbia also offer implant procedures at reduced rates for qualifying patients, which can be a practical alternative for many people.
FAQs
Can You Get Free Dental Implants Through Medicaid?
Free dental implants through Medicaid are rarely possible for adults, though children under 21 may qualify through EPSDT, and adults with reconstructive needs following illness or injury sometimes have a case worth pursuing.
For most adult enrollees, implants aren’t covered, but dental school clinics can be a practical, lower-cost alternative if you’ve been denied.
What Proof Do You Need for Medicaid to Cover Dental Implants?
Your best chance of approval generally requires a letter of medical necessity from a dentist or oral surgeon, supporting physician documentation if the tooth loss is tied to a medical condition, and evidence that conventional alternatives like dentures or bridges were considered and ruled out. Requirements vary by state, so contact your plan directly for the specific checklist before submitting.
How Much Is an Implant Out of Pocket?
A single dental implant typically costs $3,000 to $6,000, while full-mouth solutions can reach $15,000 to $30,000 or more. Dental schools often offer implants at 40 to 60 percent below market rates, and the HRSA Health Center Finder can help you locate a low-cost provider nearby.
Conclusion
Does Medicaid pay for dental implants? In most states and for most adults, the answer is no. Implants are considered elective, and state Medicaid programs typically steer enrollees toward less expensive alternatives like dentures or bridges.
Exceptions exist, particularly for children under 21, patients with congenital conditions, and those undergoing reconstructive care after cancer treatment.
If you believe your situation qualifies, work with your dental provider to build a strong medical necessity case and submit a formal prior authorization request.
If Medicaid will not cover implants, dental schools, FQHCs, and payment plans remain viable paths toward affordable tooth replacement.