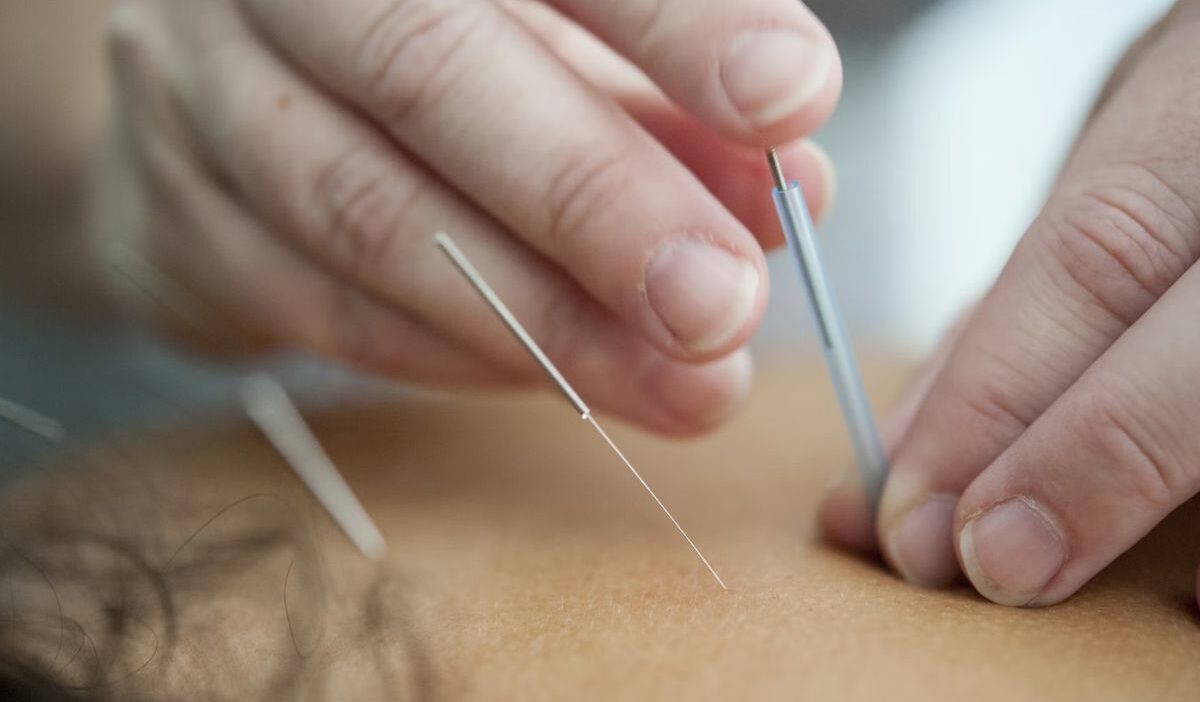
You try stretching, over-the-counter meds, maybe even physical therapy, but the pain keeps coming back. Someone suggests acupuncture, and suddenly it feels like a real option. Then the practical question shows up: is this something you can actually afford?
That’s when people start searching does Medicaid cover acupuncture, hoping for a clear answer. The reality is that a bit of layered coverage exists, but only under specific conditions.
1. Does Medicaid Cover Acupuncture in General
When acupuncture may be covered
In certain situations, the question does Medicaid cover acupuncture can be answered with yes, but only when it is considered medically necessary.
Coverage is more likely when:
- Acupuncture is used to treat chronic pain (especially lower back pain)
- A licensed provider prescribes it as part of a treatment plan
- The service follows state-approved guidelines
This reflects a broader pattern: Medicaid supports treatments that have clinical justification and measurable outcomes.
When it is not covered
Acupuncture is often not covered when it is used for:
- General wellness or relaxation
- Preventive care without a diagnosis
- Alternative therapy without medical referral
So while acupuncture may feel helpful, Medicaid typically requires a clear medical purpose before approving it.
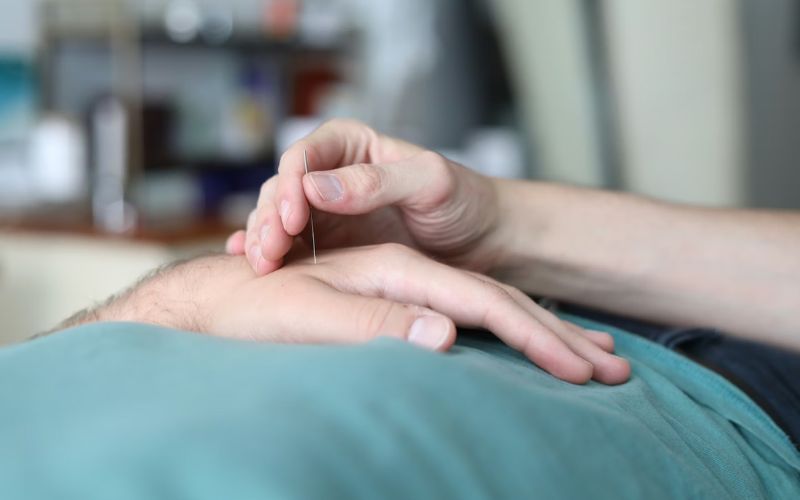
2. How Medicaid Determines Coverage for Acupuncture
To fully understand does Medicaid cover acupuncture, you need to look at how Medicaid evaluates treatments step by step, not just what the service is, but how it fits into a medical system.
Medicaid doesn’t approve acupuncture based on preference. It approves it based on structure, evidence, and necessity. Three key factors work together:
- Medical necessity
This is always the starting point. Medicaid requires a documented diagnosis, most commonly chronic pain conditions like lower back pain. But it’s not just about having a diagnosis.
- Evidence-based use
Even with a diagnosis, not every use of acupuncture is automatically covered. Medicaid looks at whether the treatment is supported by clinical evidence for that specific condition.
- Provider qualifications
The person performing the treatment matters just as much as the treatment itself. Medicaid typically requires acupuncture to be performed by a licensed practitioner who meets state and program-specific standards.
>>> Read more: Does Medicaid Cover DNA Testing? Prenatal And Pregnancy Coverage Easy Explained
3. Does Medicaid Cover Acupuncture by State
Does Medicaid cover acupuncture in NY
If you’re asking does Medicaid cover acupuncture in NY, the answer is generally yes, but with clear limits. New York Medicaid covers acupuncture primarily for chronic pain conditions, especially lower back pain.
Coverage usually requires:
- A documented diagnosis
- Treatment from a licensed acupuncturist enrolled in Medicaid
- A limited number of sessions within a defined period
This means acupuncture is treated as part of a structured pain management plan, not a general wellness service.
Does Medicaid cover acupuncture in NYC
For those wondering, does Medicaid cover acupuncture in NYC, the rules are the same as New York State, but access can differ slightly due to provider availability.
In practice:
- More clinics in NYC accept Medicaid for acupuncture
- Wait times may vary depending on demand
- Coverage still depends on medical necessity and approved conditions
So while availability may be better in a large city, the eligibility criteria remain unchanged.

Does Medicaid cover acupuncture in Colorado
When looking at does Medicaid cover acupuncture in Colorado, coverage exists but in limited cases. Colorado Medicaid may include acupuncture for pain management, especially when recommended by a healthcare provider.
However:
- Not all conditions are covered
- Session limits may apply
- Some plans require prior authorization
This creates a system where acupuncture is available, but only when it fits clearly into a treatment plan.
Does Medicaid cover acupuncture in Virginia
If you’re asking, does Medicaid cover acupuncture in Virginia, the answer is more limited. Virginia Medicaid generally does not include acupuncture as a standard benefit, although limited coverage may exist under specific plans or programs.
In some cases:
- Coverage may exist through specific programs or pilot initiatives
- Patients may need referrals or additional approval
- Out-of-pocket payment is more common compared to other states
This highlights an important contrast: even when the same question does Medicaid cover acupuncture is asked, the outcome can be very different depending on location.
4. How to Check If Your Plan Covers Acupuncture
Step 1: Call your Medicaid provider directly
Start by contacting your Medicaid plan using the number on your insurance card. Instead of asking a general question, be specific: ask whether acupuncture is covered, for which conditions, how many sessions are allowed, and whether prior authorization is required.
Step 2: Consult your primary care doctor
Your doctor plays a key role in turning acupuncture into a medically necessary service. Explain your symptoms clearly, especially if you’re dealing with chronic pain or functional limitations.
Step 3: Check your state Medicaid website
Each state publishes its own list of covered services. Look under sections like “pain management,” “behavioral health,” or “alternative therapies.” Pay attention to details such as eligible conditions, provider requirements, and session limits.
Step 4: Ask the acupuncture clinic directly
Many clinics already work with Medicaid patients and understand the billing process. Ask if they accept your specific plan, whether they handle prior authorization, and what documentation is needed.
>>> Read more: Does Medicaid Cover Vyvanse? Adult And Generic Coverage Easy Explained
5. Alternatives if Acupuncture Is Not Covered
Physical therapy
Physical therapy is one of the most reliable alternatives if Medicaid does not cover acupuncture turns out to be limited in your plan.
Medicaid often fully covers physical therapy when it’s prescribed for pain, injury recovery, or mobility issues.
Chiropractic care (in some states)
In certain states, chiropractic services are included under Medicaid benefits. If you’re exploring options beyond acupuncture, this can be a practical path.
Chiropractic care targets spinal alignment and musculoskeletal pain, which overlaps with conditions people often seek acupuncture for.
Community health programs
Some nonprofit clinics and community health centers offer low-cost or sliding-scale acupuncture services. These programs are especially helpful when Medicaid does not cover acupuncture directly.
Pain management clinics
Pain management clinics offer comprehensive treatment plans that may include physical therapy, medication, behavioral therapy, or other approved services.
Medicaid is more likely to cover these programs because they follow a structured, clinical approach.
6. FAQs
Does Medicaid cover acupuncture in all states?
No. Medicaid coverage for acupuncture varies by state. Some states include it for specific conditions like chronic pain, while others do not cover it at all or only in limited programs.
How many sessions does Medicaid cover?
The number of sessions depends on your state and condition. When acupuncture is covered under Medicaid, plans often limit visits per year or require ongoing evaluation to continue treatment.
Is acupuncture considered a medical treatment?
Sometimes. It is considered medical treatment when used for a diagnosed condition and prescribed as part of a care plan. Otherwise, it is often viewed as alternative care and may not be covered.
Conclusion
Understanding does Medicaid cover acupuncture helps you focus on what actually works within your plan instead of guessing. The key is to align acupuncture with medical necessity, confirm your state’s rules, and choose the right provider from the start.
Before booking any session, take a few minutes to check your coverage, ask your doctor for guidance, and verify approved clinics. These simple steps can help you access treatment faster while avoiding unexpected costs.