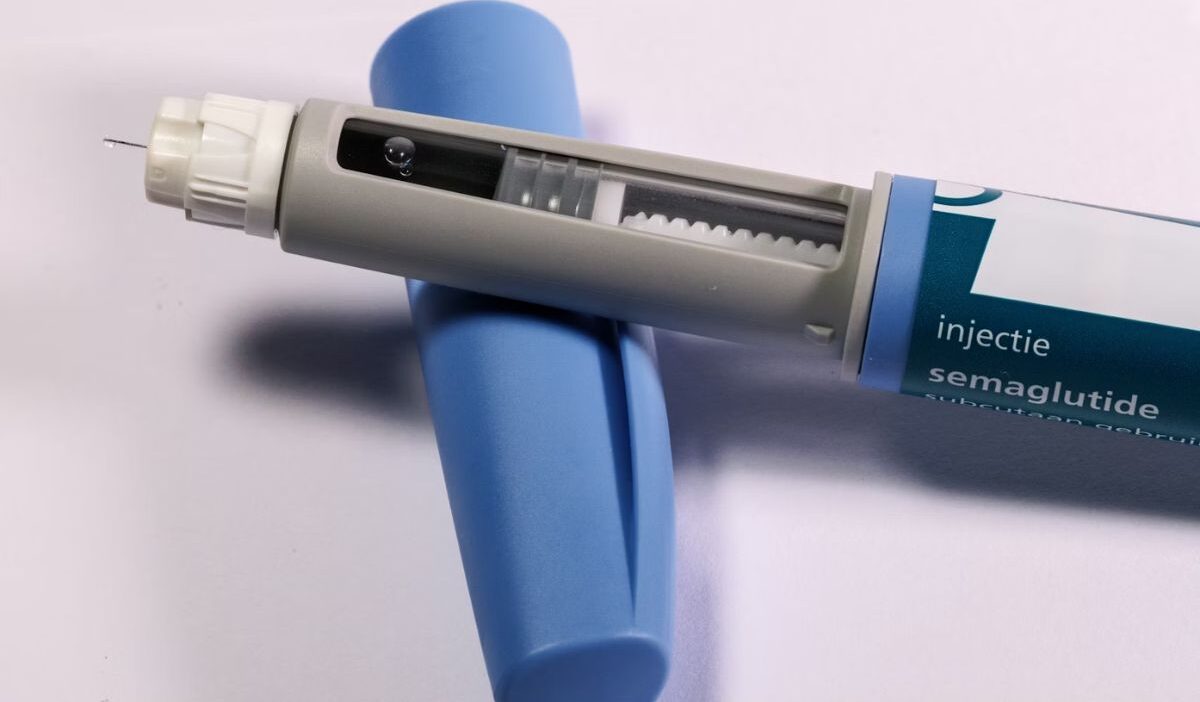
You start noticing the pattern of blood sugar creeping up, weight harder to manage, and energy dropping faster than before. Your doctor mentions Ozempic, and suddenly it feels like a real solution.
So the next step is obvious: searching does Medicaid cover Ozempic to see if it’s even an option. The answer exists, but it depends on why you need it, where you live, and how it’s prescribed.
1. Does Medicaid Cover Ozempic in General
The short answer to does Medicaid cover Ozempic? is: Medicaid may cover Ozempic, but approval usually depends on diagnosis, medical necessity, and state-specific plan rules.
Ozempic is primarily approved for treating type 2 diabetes, and Medicaid coverage usually follows that purpose. If your doctor prescribes it to control blood sugar and improve long-term health outcomes, coverage is much more likely.
However, Medicaid does not automatically approve every prescription. It typically requires:
- A confirmed diagnosis of type 2 diabetes
- Medical documentation showing the need
- Sometimes prior authorization
This creates a cause-and-effect structure: When Ozempic is used as a medical treatment, coverage is possible. When it’s used outside that scope, approval becomes harder.
2. Does Medicaid Cover Ozempic for Different Conditions
Does Medicaid cover Ozempic for weight loss
This is where expectations often don’t match reality. If you’re asking, does Medicaid cover Ozempic for weight loss? The answer is usually no.
Even though Ozempic can lead to weight loss, Medicaid typically does not cover it for that purpose alone. Weight loss is often classified as non-essential unless tied to a serious medical condition.
So:
- Weight loss alone → usually not covered
- Weight loss tied to diabetes → may be covered indirectly
This distinction explains why two people taking the same medication can receive completely different coverage decisions.
Does Medicaid cover Ozempic for prediabetes
When it comes to does Medicaid cover Ozempic for prediabetes, coverage is less common.
Prediabetes is considered a risk condition, not a confirmed disease. Coverage for prediabetes is generally less common because Ozempic is usually approved within type 2 diabetes treatment criteria.
That said, some providers may still attempt approval if:
- Risk factors are severe
- Other treatments have failed
- The case is medically justified
But overall, approval remains limited.
>>> Read more: Does Medicaid Pay For Liposuction? What You Need To Know in 2026
3. Does Illinois Medicaid Cover Ozempic
If you’re specifically asking, does Illinois Medicaid cover Ozempic? The answer is yes, but only when strict medical criteria are met. Illinois Medicaid does not treat Ozempic as a general-use medication. Instead, it follows a structured approval system designed to control costs and ensure appropriate use.
Illinois Medicaid plans may require step therapy or prior authorization before approving Ozempic.
First, Ozempic must be prescribed for type 2 diabetes, not for weight loss or general health improvement. This is the foundation of coverage. Without a confirmed diagnosis, approval is very unlikely.
Second, Illinois typically applies a step therapy approach. This means:
- Patients are often required to try first-line medications (like metformin)
- Ozempic is considered only if those treatments are ineffective or not tolerated
Third, prior authorization is usually required. Your healthcare provider must submit:
- Medical records confirming diagnosis
- History of previous treatments
- Justification for why Ozempic is necessary
4. Does NC Medicaid Cover Ozempic
For those wondering does NC Medicaid cover Ozempic? The structure is similar but with its own state-specific rules. North Carolina Medicaid plans may cover Ozempic for type 2 diabetes, subject to medical necessity and plan requirements.
Coverage is generally approved when:
- The patient has a confirmed diagnosis of type 2 diabetes
- Blood sugar levels are not well-managed with standard treatments
- A provider submits proper documentation and prior authorization
Like Illinois, North Carolina also emphasizes medical necessity over preference. That means Ozempic is not typically approved as a first-line treatment. Instead, it becomes an option when other medications have not delivered results.
If you’re asking, does Medicaid cover Ozempic in North Carolina for weight loss, the answer is usually no. Even though Ozempic is widely known for its weight-related benefits, Medicaid evaluates it strictly within a clinical diabetes framework.
>>> Read more: What Does Medicaid Not Cover In NY? Coverage Limits Explained
5. How to Get Ozempic Approved Under Medicaid
Step 1: Get a confirmed diagnosis of type 2 diabetes
The first and most important step is having a clear, documented diagnosis. Medicaid typically only approves Ozempic when it is used to treat type 2 diabetes, not for general weight loss. Your doctor must provide medical records, lab results (like A1C levels), and evidence that your condition requires treatment.
Step 2: Follow step therapy requirements
Most Medicaid plans require patients to try standard, lower-cost medications before approving Ozempic. This is known as step therapy. For example, you may need to show that medications like metformin were ineffective or caused side effects.
Step 3: Submit prior authorization through your provider
Even with the right diagnosis, approval is not automatic. Your healthcare provider must submit a prior authorization request that includes your treatment history, current condition, and justification for Ozempic.
Step 4: Use Medicaid-approved providers and pharmacies
To ensure coverage, both your doctor and pharmacy must be enrolled with Medicaid. If not, the prescription may be denied even if you meet all medical criteria. Choosing approved providers helps avoid delays, reduces paperwork issues, and increases your chances of getting Ozempic covered successfully.
6. FAQs
Does Medicaid cover Ozempic for everyone?
No. Medicaid coverage for Ozempic depends on medical necessity, diagnosis (usually type 2 diabetes), and state-specific rules; not everyone qualifies.
Is Ozempic free with Medicaid?
Not always. It can be low-cost or free depending on your plan, but some copays or approval conditions may still apply.
Can Ozempic be covered for weight loss?
Usually no. Medicaid coverage for Ozempic for weight loss is typically not available unless it’s tied to a diagnosed medical condition like type 2 diabetes.
Conclusion
Understanding does Medicaid cover Ozempic gives you a clear advantage when navigating treatment options. The real benefit is knowing what documentation and medical criteria Medicaid may require, so it aligns with the requirements.
Before moving forward, confirm your diagnosis, talk with your doctor about eligibility, and check your state plan details. Taking these steps early can help you get approved faster and avoid delays or unexpected costs when accessing Ozempic.