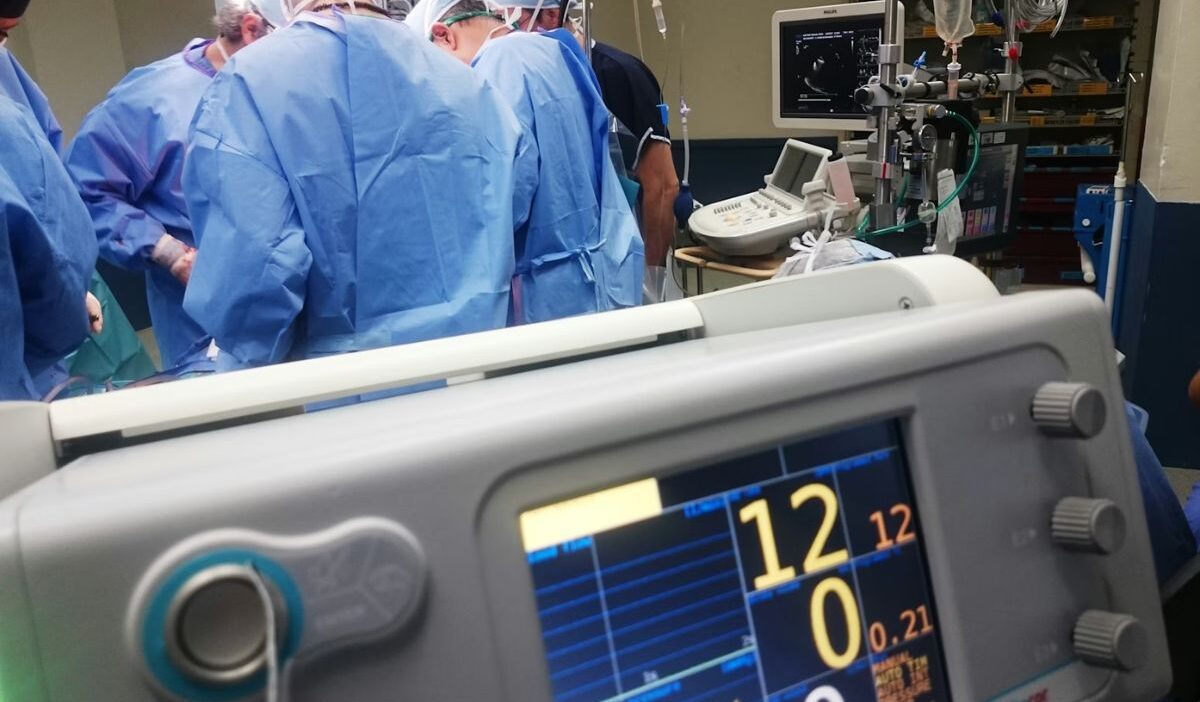
It’s the kind of moment you don’t plan for. A sudden injury, sharp chest pain, or a child with a high fever late at night, you go straight to the ER without thinking twice.
That’s when people start searching does Medicaid cover emergency room visits, trying to understand what’s actually covered and what isn’t. The good news: coverage exists. The challenge: knowing when it applies.
1. Does Medicaid Cover Emergency Room Visits in General
What qualifies as an emergency
In most cases, does Medicaid cover emergency room visits depends on whether the situation meets the definition of an emergency.
An emergency is typically defined as a condition with:
- Severe pain
- Risk to life or health
- Need for immediate medical attention
For example, symptoms like chest pain, difficulty breathing, serious injury, or sudden neurological issues usually qualify. This definition matters because Medicaid uses it as the primary filter for coverage.
What is usually covered
When the visit meets emergency criteria, Medicaid generally covers:
- ER evaluation and treatment
- Diagnostic tests (X-rays, blood work)
- Emergency procedures
- Stabilization care
This reflects a clear cause–and–effect structure: If the condition is urgent and medically necessary, coverage is highly likely.
What Medicaid may not fully cover
Not every ER visit is treated the same. If the issue is considered non-emergency, such as minor symptoms that could be handled at urgent care, coverage may be limited.
In those cases:
- You may face partial payment
- Claims may be reviewed or denied
- Follow-up care may not be included
This is where confusion often happens when asking does Medicaid cover emergency room visits, because the answer depends on how the visit is classified.

2. Other Medicaid ER Inquiries
- Does Medicaid cover out of state emergency room visits
Yes, in genuine emergencies, Medicaid will generally cover an out-of-state emergency room visit. Federal guidelines require Medicaid programs to pay for emergency care regardless of where it occurs, as long as the situation meets the definition of a medical emergency.
- Does Medicaid cover emergency room visits out of state
Yes, if the situation is a true emergency, Medicaid will generally cover an out-of-state emergency room visit. The program is designed so that when your condition is serious and needs immediate attention, you can receive care wherever you are, not just in your home state.
If something urgent happens while you are away, it is completely understandable to feel unsure about what will be covered. In that moment, the priority is simple: get the care you need right away. Your health comes first, and those protections are there so you are not left without help when it matters most.
- Does Illinois Medicaid cover out of state emergency room visits
If you are wondering specifically about Illinois Medicaid, the answer follows that same principle. Emergency treatment is typically covered, even outside the state.
At the same time, services that are not urgent, or any care that continues after the emergency has been handled, are usually expected to take place within Illinois and may not be covered the same way.
- Does Medicaid cover emergency room visits without insurance card
Yes, even if you do not have your Medicaid card with you at the time, your emergency room visit can still be covered as long as you are enrolled. Hospitals have ways to confirm your eligibility afterward, and once your information is verified, the visit can be billed to Medicaid instead of you having to pay out of pocket.
- Does pregnancy Medicaid cover emergency room visits
Yes, in most cases, pregnancy Medicaid does cover emergency room visits. When the situation is urgent, especially if it involves complications or symptoms that could affect the health of the mother or the baby, that care is considered essential and is typically covered.
If you are expecting and something does not feel right, it is natural to worry about both your health and your coverage. In those moments, trust your instincts and seek care right away. The support is there so you can focus on staying safe and getting the attention you and your baby need.

3. How to Ensure Your ER Visit Is Covered
- Use the ER only for true emergencies
Choosing the ER for situations that genuinely require immediate care is the most important factor. Medicaid evaluates whether your condition meets emergency criteria, so severe symptoms like chest pain, breathing difficulty, or serious injury are more likely to be fully covered.
- Describe symptoms clearly and accurately
When speaking with medical staff, explain your symptoms in detail, when they started, how severe they are, and how they impact you. Accurate descriptions help providers record the medically necessary, which supports approval when determining does Medicaid cover emergency room visits.
- Follow up with in-network providers
After your ER visit, additional care such as tests, specialist visits, or prescriptions may be needed. Medicaid often requires follow-up care to be done with in-network providers to maintain coverage.
- Keep documentation from your visit
Always keep discharge papers, test results, and any billing statements you receive. These documents are important if there are questions about your claim or if Medicaid needs additional information.
>>> Read more: Does Urgent Care Take Medicaid? 4 Documents Must Bring
4. FAQs
Does Medicaid cover all emergency room visits?
No. Medicaid coverage for emergency room visits depends on whether the situation is considered a true emergency. Non-urgent visits may be only partially covered or denied.
Does Medicaid cover emergency room visits out of state automatically?
In most cases, yes, Medicaid will cover out-of-state emergency room visits when immediate medical care is needed. Emergency situations are generally handled regardless of location, as long as the condition requires urgent attention.
However, services that are not considered emergencies are typically not covered outside your home state. It is always a good idea to check with your specific Medicaid plan if you are unsure about coverage beyond emergency care.
Is ER care free with Medicaid?
Not always. Emergency room visits are often covered at little to no cost, but this can vary depending on your specific Medicaid plan. In some cases, small copays or limited charges may still apply.
Conclusion
Understanding does Medicaid cover emergency room visits helps you make faster, smarter decisions in urgent situations. The key benefit is knowing when your visit qualifies, so you can act without second-guessing coverage.
When an emergency happens, focus on getting care first. After that, make sure your visit aligns with Medicaid guidelines, keep your records, and follow up properly. That way, you protect both your health and your coverage at the same time.