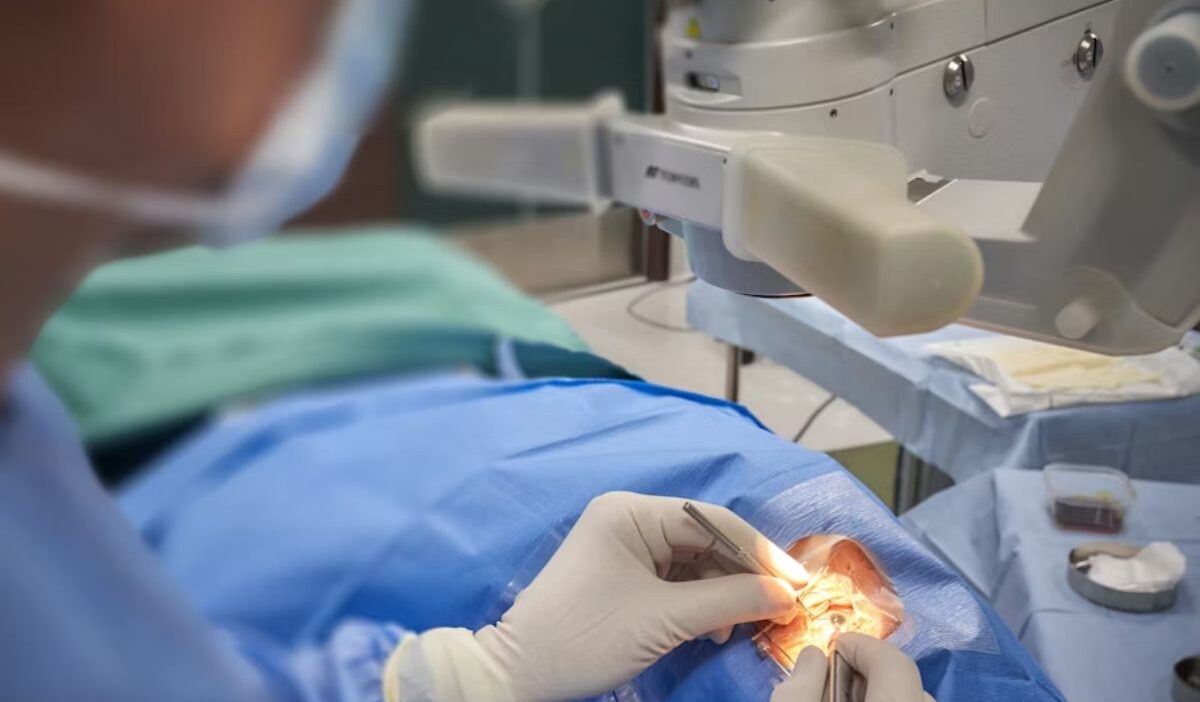
Vision changes often happen gradually. At first, it’s just a bit of blur or difficulty seeing at night. Over time, everyday tasks like reading, driving, or recognizing faces become harder.
When a doctor mentions cataract surgery, the next concern is usually cost. For many individuals relying on Medicaid, this leads to an important question about coverage and eligibility.
1. Does Medicaid Cover Cataract Surgery in General
When surgery is covered
In most cases, does Medicaid cover cataract surgery has a reassuring answer: yes, when it is considered medically necessary.
Cataract surgery is typically covered when:
- Vision impairment affects daily activities like driving or reading
- An eye doctor confirms reduced visual acuity
- Surgery is required to restore functional vision
This reflects how Medicaid works: it prioritizes treatments that restore essential health functions, not just improve comfort.
When coverage may be limited
However, coverage is not unlimited. Medicaid may restrict or partially cover certain aspects, especially when the procedure goes beyond basic medical needs.
Limitations often include:
- Premium intraocular lenses (IOLs)
- Advanced surgical techniques chosen for convenience or customization
- Non-essential upgrades that improve vision quality beyond standard correction
So, while does Medicaid cover cataract surgery is generally yes, the type of surgery matters just as much as the need for it.
2. Does Medicaid Cover Cataract Surgery for Seniors
For older adults, the question does Medicaid cover cataract surgery for seniors comes up frequently, and the answer is largely favorable.
Seniors are more likely to qualify because:
- Cataracts are age-related and medically recognized
- Vision decline directly impacts independence and safety
- Surgery is considered a necessary intervention, not elective
If a senior meets medical criteria, Medicaid typically covers:
- Pre-surgical eye exams
- Standard cataract removal procedure
- Basic intraocular lens implantation
For seniors who qualify for both Medicaid and Medicare (dual eligibility), the two programs may work together to expand coverage.
>>> Read more: Does Medicaid Cover Glasses? Easy Guide 2026
3. Does Medicaid Cover Laser Cataract Surgery
This is where confusion often happens. People hear about newer techniques and ask: Does Medicaid cover laser cataract surgery?
The answer is more nuanced.
Standard cataract surgery is generally covered because it is well-established, effective, and cost-efficient. In contrast, laser-assisted methods are often viewed as an enhanced option rather than a necessity.
In practice, this means:
- Medicaid typically pays for the cost of the standard procedure
- Any added cost related to laser technology may be the patient’s responsibility
The distinction is quite simple:
- Medically necessary treatment is usually covered
- Optional technology upgrades may be only partially covered or not included
While laser-assisted surgery can provide added precision, it is not always fully covered under Medicaid plans.
4. How to Qualify for Cataract Surgery Under Medicaid
- Get a confirmed diagnosis from an eye specialist
An ophthalmologist must verify that you have cataracts and that your vision is significantly affected. This step is critical because Medicaid only considers coverage when there is clear medical evidence, not just general discomfort or mild symptoms.
- Show that vision loss affects daily activities
Medicaid looks beyond test results and focuses on real-life impact. Difficulty driving, reading, working, or recognizing faces can support medical necessity. The stronger the link between vision loss and daily limitations, the more likely approval becomes.
- Complete required approvals or referrals
Many Medicaid plans require prior authorization before surgery. Your provider will submit medical records and justification for the procedure. This ensures the treatment meets coverage criteria and avoids unexpected denials later.
- Use a Medicaid-approved provider and facility
Even if you qualify medically, the surgery must be performed by a provider who accepts Medicaid. Choosing an in-network surgeon and clinic helps ensure the procedure is covered and prevents additional out-of-pocket costs.
5. FAQs
Does Medicaid cover cataract surgery in all states?
Not always. Medicaid is a state-run program, so coverage can vary. Most states do cover cataract surgery when it is medically necessary, but the exact requirements, approvals, and benefits may differ. Always check your state’s Medicaid plan for details.
Does Illinois Medicaid cover cataract surgery?
Yes, Illinois Medicaid may cover cataract surgery if it is medically necessary. A doctor must confirm the need, and prior authorization may be required. Basic surgery is typically covered, while premium lens upgrades may cost extra. Coverage can vary, so check with your provider.
Does Indiana Medicaid cover cataract surgery?
Yes, Indiana Medicaid generally covers cataract surgery when it is medically necessary. An eye care professional will need to evaluate your condition and recommend the procedure.
While the standard surgery is typically included, upgraded lens options or elective services may not be covered. Because coverage can vary by plan, it’s a good idea to check with your Medicaid provider for specific details.
Is cataract surgery free with Medicaid?
It can be low-cost or fully covered if it’s medically necessary, but it’s not always completely free. Some plans may include small copays, and optional upgrades (like premium lenses) are usually not covered. Coverage varies by state and plan.
Does Medicaid cover laser cataract surgery fully?
Not usually. Medicaid typically covers standard cataract surgery, while laser-assisted procedures are often considered optional and may require out-of-pocket costs. Coverage varies by state and plan.
Conclusion
Understanding does Medicaid cover cataract surgery helps you avoid confusion and choose the right path from the start. The key benefit is knowing the Medicaid requirements, so you don’t waste time on services that won’t be covered.
If you’re planning to seek support:
- Check your Medicaid plan details
- Speak with a licensed provider about medically necessary options
- Ask how sessions can be structured to qualify for coverage
Taking these steps can help you access the care you need more efficiently, while making sure your benefits are actually used the right way.